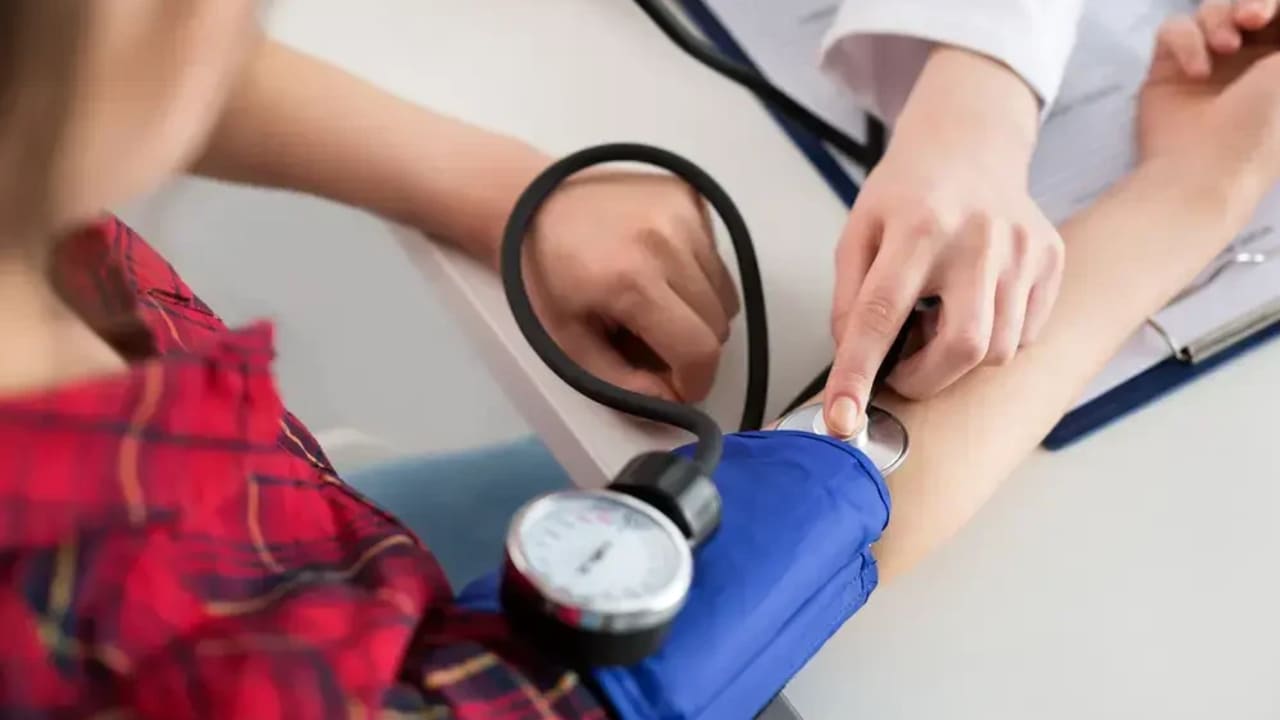
Stopping eating a few hours before bedtime has gained attention in recent years as a simple strategy that may support blood pressure balance, blood sugar levels, and heart health in general. The combination of avoiding nighttime eating and eating within a defined time window (Time-Restricted Eating) highlights how much meal timing affects the biological clock and the cardio-metabolic system.
In an article on the Medical Daily website, it was explained that this is not a “magic method,” but rather a gradual approach that seeks to align nutrition, sleep, and metabolism.
Many professionals recommend leaving a gap of at least two to three hours between the last meal and bedtime. A three-hour gap allows the body to digest the meal, reduce the post-meal rise in blood sugar levels, and gradually enter a state of rest and nighttime repair.
When meal timing is adjusted to this natural rhythm, the heart and blood vessels may experience less strain during the night.
Many also report less heartburn, reflux, and discomfort when lying down after they stop eating close to bedtime. Heavy or high-fat meals late at night keep the digestive system active – and sometimes impair sleep quality and nighttime recovery.
It is important to emphasize: Eating before bedtime is not “forbidden,” but quantity, composition, and consistency matter. Large meals, sugar-rich desserts, and salty, processed snacks raise blood sugar levels and may cause fluid retention. Over time, such a pattern may affect weight, metabolic markers, and heart function at night.

How does this affect blood pressure?
Eating within a defined time window is a dietary pattern in which food is consumed over 8–12 hours per day and fasting is maintained during the remaining hours. When the eating window ends at least three hours before bedtime, a longer and more consistent nighttime fast is achieved.
Blood pressure follows a daily pattern: It rises during the day and falls at night. The “nocturnal dip” is considered essential for allowing the cardiovascular system to rest. Late eating may blur this dip, as it keeps the body in an active metabolic state at a time when it is supposed to relax.
Leaving a gap of three to four hours between dinner and sleep allows post-meal peaks in blood sugar and blood pressure to pass before falling asleep. Combined with physical activity and a balanced diet, such a pattern may contribute to improved blood pressure markers over time.
Blood sugar control is closely linked to the biological clock. According to the World Health Organization, the body’s sensitivity to insulin and its ability to handle glucose are generally higher during the day and lower at night.
When large meals or sweet snacks are consumed late in the evening, blood sugar levels may remain higher and for longer compared to eating earlier in the day. Stopping food intake three hours before bedtime may allow the body to complete most of the glucose response before sleep and reduce nighttime metabolic load.
For people at risk of type 2 diabetes or those trying to improve metabolic markers, aligning meal timing with the circadian rhythm may be a significant factor. However, people with diabetes or those taking blood sugar-lowering medications should make changes under medical supervision.
Meal timing and heart health
Heart health depends not only on what you eat – but also on when. According to researchers from Harvard, the cardiovascular system, hormones, and metabolism all operate according to daily rhythms that are sensitive to light, sleep, and eating.
When most calories are consumed during daytime hours and a consistent nighttime fast is maintained, the body’s systems tend to function in a more synchronized manner. Studies indicate that shifting calories to earlier hours and eating within a limited time window may lead to moderate improvements in blood pressure, heart rate, and fasting blood sugar markers – even without a dramatic change in total calorie intake.
In addition, avoiding heavy meals before bedtime may improve sleep quality. Better sleep is associated with more balanced blood pressure, improved insulin sensitivity, and reduced inflammation – all significant factors for long-term heart health.